
Press Release Ohio Auditor of State
Special Report Details Costs, Dangers of Noncompliance in Ohio’s Medicaid Program
Pending Legislation Would Establish Additional Safeguards for State’s High-Risk Medicaid Providers
Columbus – Medicaid providers who are unqualified or lack records to justify payments for services have repaid only a fraction of the tens of millions of dollars they owe to the state, according to a released today by Auditor of State Dave Yost.
The report highlights the costs and dangers citizens face when Medicaid providers disregard the regulations put in place to prevent fraud and inadequate care. Legislation introduced in the fall with the support of Auditor Yost aims to curb these risks with tougher safeguards for high-risk providers.
“For too long, dishonest providers have exploited vulnerabilities in the Medicaid program with little consequence,” Auditor Yost said. “A stronger system of controls is necessary to protect the program’s vital resources and the citizens who need them most.”
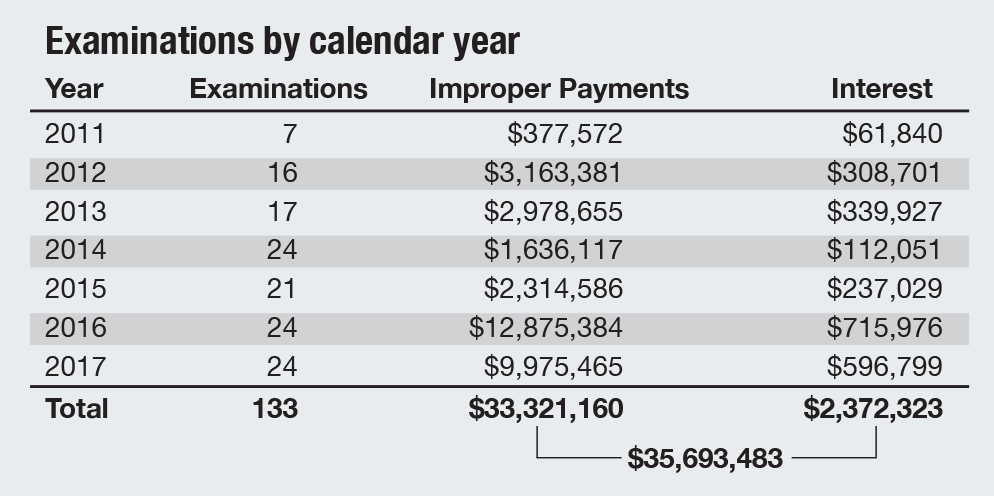
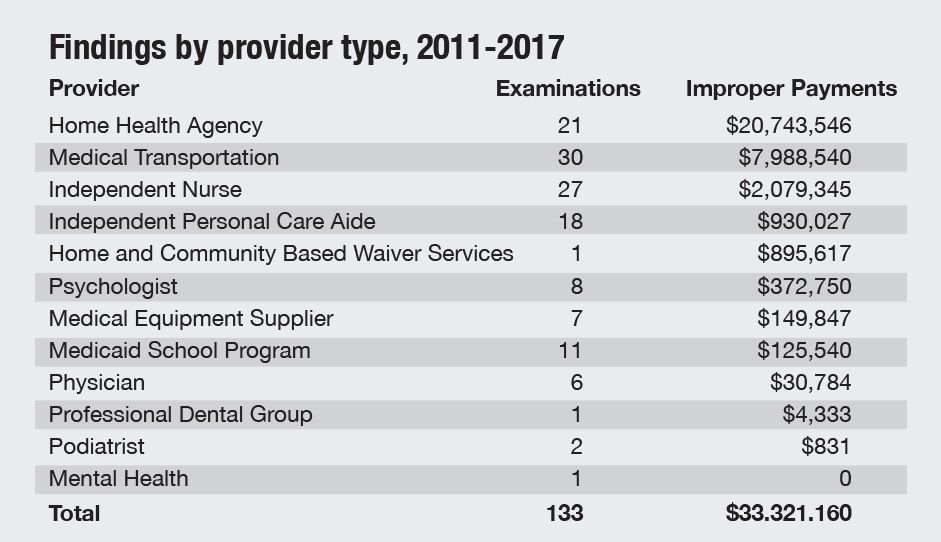
In the past seven years, the Auditor of State’s office has performed compliance examinations of 133 Medicaid providers, flagging $33.3 million in improper payments and calculating an additional $2.4 million in interest. The payments typically result from providers charging for care they are not certified to provide or for services that lack supporting documentation.
A recent follow-up analysis of 60 of those providers disclosed that they have repaid only 9.6 percent ($1.9M) of the $19.7 million they owe back to the Ohio Department of Medicaid (ODM). Most of the cases for the remaining providers are still pending.
With millions of users and more than 110,000 active providers, Ohio’s Medicaid program accounts for the largest share of the state’s financial resources with 39.3 percent of all fund appropriations earmarked for Medicaid spending in the 2018-19 biennium. In 2016 alone, ODM paid business and individual care providers $22.3 billion for their services.
The special report, Ohioans at Risk: Noncompliance in Ohio’s Medicaid Program Poses Dangers, Wastes Tax Dollars, is part of Auditor Yost’s continued efforts to foster a culture of accountability in state and local government. Those efforts include work on Senate Bill 218, introduced in October by Sen. Peggy Lehner, to target providers that are at the greatest risk for improper billings.
While transportation and home health providers only make up between 13 and 17 percent of the total providers in the Medicaid program, they account for more than 86 percent ($28.7 million) of the $33.3 million in overpayments identified since 2011.
The bill, which awaits its first committee hearing, would require these types of providers to obtain surety bonds that would help the state recover losses caused by fraud and improper payments. Indiana, Texas, Florida and New York use a similar approach.
It also would require them to complete training in billing, records retention and Medicaid compliance before becoming certified to provide Medicaid services. According to the report, both areas of the Medicaid program have shown signs of rapid growth in recent years and have minimum qualification requirements compared to other types of providers.
“Make no mistake, transportation and home health providers deliver critical services that countless Ohioans rely on every single day,” Auditor Yost said. “But limited safeguards for these fields have given rise to widespread abuse and improper billing costing tens of millions of dollars.”
You can check out an interactive map of improper payments uncovered during Auditor of State compliance examinations.

###
The Auditor of State’s office, one of five independently elected statewide offices in Ohio, is responsible for auditing more than 5,900 state and local government agencies. Under the direction of Auditor Dave Yost, the office also provides financial services to local governments, investigates and prevents fraud in public agencies and promotes transparency in government.
Contact:
Press Secretary
614-644-1111